Ambulance vs. Non-Emergency Medical Transport: When Rapid Wheelchair & Stretcher Services Are the Smarter Choice
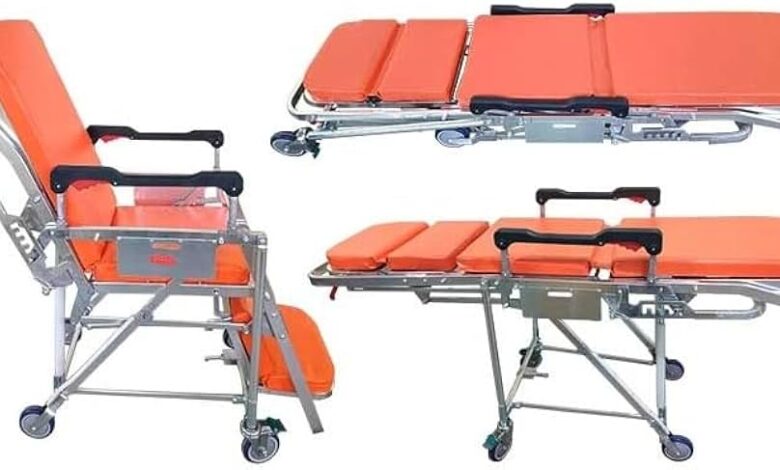
When someone needs to get to a medical appointment, dialysis session, post-surgical follow-up, or discharge from a hospital, the question of how they travel is rarely treated as a serious operational decision. Most families, care coordinators, and discharge planners default to the most familiar option — calling an ambulance — without considering whether that level of response is actually appropriate for the situation. The result is often unnecessary cost, strained emergency resources, and a transport experience that creates more stress than it relieves.
This distinction matters in real care environments. Emergency medical services are designed for acute, life-threatening situations. When they are used for routine or scheduled medical transport, particularly for patients with mobility limitations, the outcome is rarely efficient for anyone involved — not the patient, not the care facility, and not the broader emergency system. Understanding where the line falls between emergency and non-emergency transport, and what purpose-built non-emergency services actually offer, is a practical necessity for anyone involved in coordinating patient movement.
What Non-Emergency Medical Transport Actually Covers
Non-emergency medical transport (NEMT) refers to scheduled, medically necessary transportation provided to patients who cannot use standard transit or private vehicles due to a physical condition, mobility limitation, or medical need that requires supervised handling. This category is broader than most people assume. It includes patients using manual or power wheelchairs, those transported on stretchers due to post-surgical recovery or chronic conditions, and individuals who require positioning support, oxygen, or monitoring during travel — but who do not require paramedic-level emergency intervention.
Within this space, rapid wheelchair & stretcher transport has emerged as a defined service category for patients who need timely, dignified, and medically appropriate transport without triggering emergency protocols. You can review how this type of service is structured and deployed at providers like rapid wheelchair & stretcher transport. The key distinction from ambulance services is that these transports are planned, coordinated in advance or dispatched quickly within a non-emergency framework, and staffed by trained transport professionals rather than paramedics or emergency medical technicians responding to crises.
For care coordinators and discharge teams, this matters because the transport itself must match the clinical and logistical reality of the patient. Placing a stable patient who uses a wheelchair into an ambulance because no other option was arranged is a failure of planning, not a clinical necessity. Purpose-built NEMT services are designed to fill this gap systematically.
The Patient Profile That Drives Demand for This Service
The patients who benefit most from rapid wheelchair and stretcher transport are those whose conditions are stable but whose mobility is significantly limited. This includes individuals recovering from orthopedic surgery who cannot bear weight, dialysis patients who attend multiple appointments per week, residents of long-term care facilities who require transport for diagnostic imaging or specialist consultations, and patients discharged from hospitals who are not yet mobile enough to sit upright in a standard vehicle.
What these patients share is not a medical emergency — it is a physical reality that requires equipment, trained handling, and a transport environment designed to accommodate their condition safely. When this need is met by an ambulance, the patient often receives a higher level of service than required, at a significantly higher cost, while occupying a resource that exists for acute emergencies. When it is met by an unequipped vehicle or a family member with no training in proper transfer technique, the risk of injury during loading, transit, or unloading increases substantially.
How Ambulance Services Are Designed — and Where That Design Ends
Ambulance services operate within emergency medical systems governed by protocols, dispatch priorities, and clinical standards designed around time-critical situations. According to the Centers for Medicare and Medicaid Services, ambulance transport is covered under specific medical necessity criteria, and that necessity is assessed based on whether the patient’s condition requires on-scene emergency response or advanced life support during transit. Routine transport does not meet this threshold, which is precisely why NEMT exists as a separate, funded category.
The clinical staff on ambulances — paramedics and emergency medical technicians — are trained to stabilize, assess, and intervene in acute situations. Their equipment reflects this purpose: cardiac monitors, defibrillators, IV administration, airway management tools. When a patient simply needs safe transport in a reclined or wheelchair position without clinical intervention, deploying this level of resource is operationally misaligned. It occupies an ambulance unit, requires emergency documentation, and often places the patient in an environment optimized for crisis rather than comfort or routine care.
Cost Implications That Often Go Unexamined
One of the most consistent gaps in transport planning is the assumption that ambulance services and non-emergency transport cost roughly the same, or that insurance will simply cover whatever is used. In practice, ambulance transport for non-emergency situations is frequently denied by insurance, Medicare, or Medicaid when medical necessity cannot be documented to the required standard. Patients and families often discover this only after the fact, when a bill arrives for a transport that could have been handled through a covered NEMT benefit at a fraction of the cost.
Non-emergency medical transport, including rapid wheelchair and stretcher options, is explicitly covered under Medicaid in all U.S. states as a required benefit when the transport is medically necessary and the patient cannot use other modes of transit. Many Medicare Advantage plans and private insurance policies include similar provisions. The financial argument for using the appropriate transport level is not about cutting corners — it is about ensuring that the right claim is submitted for the right service, which protects both the patient and the care organization from avoidable billing complications.
Response Time and Scheduling: A Practical Comparison
One of the reasons ambulances are reflexively called for mobility-limited patients is the assumption that they respond faster or more reliably than NEMT providers. This assumption is often incorrect in practice. Emergency dispatch prioritizes calls by acuity, which means a non-emergency patient calling for an ambulance may wait significantly longer than someone with a confirmed life-threatening event — and rightly so. Meanwhile, NEMT providers operating within a rapid-dispatch model can often reach a patient for a scheduled or same-day transport within a timeframe comparable to, or faster than, waiting for a non-priority ambulance deployment.
Rapid wheelchair & stretcher transport services, when properly staffed and dispatched, are built around the specific logistical needs of time-sensitive but non-acute transport. Discharge windows, appointment slots, and dialysis schedules do not accommodate multi-hour waits. NEMT providers that specialize in this segment have invested in dispatch infrastructure and vehicle availability precisely because the patient population they serve has recurring, predictable, and time-dependent needs.
Consistency Across Repeated Transports
For patients with chronic conditions or recovery trajectories that require regular transport over weeks or months, consistency is not a secondary concern — it is a clinical and safety one. A dialysis patient who is transported three times per week benefits significantly from a service that maintains familiarity with their equipment, transfer preferences, positioning requirements, and medical history notes. Ambulance services cannot offer this continuity because they are not structured around recurring non-emergency relationships with individual patients.
NEMT providers focused on wheelchair and stretcher transport can build operational familiarity with patients over time. This reduces transfer errors, improves patient comfort, and allows transport staff to flag changes in condition that may be clinically relevant. That kind of continuity represents a meaningful layer of informal safety monitoring that adds real value to care coordination, without requiring clinical intervention.
How Discharge Planners and Care Coordinators Should Think About This Decision
Hospital discharge planning and care coordination teams bear a disproportionate share of responsibility for transport decisions, often under significant time pressure. The temptation to call an ambulance as the default safe choice is understandable, but it reflects risk aversion rather than clinical judgment. The appropriate framework is straightforward: does this patient require emergency medical intervention during transit, or do they require a safe, equipped, and supervised transport environment?
If the answer is the latter, then rapid wheelchair & stretcher transport is not a compromise — it is the clinically and operationally appropriate choice. Documenting this decision clearly, verifying coverage in advance, and selecting a provider with a clear safety and training record protects the care team, the patient, and the organization from liability and financial exposure.
Care facilities that establish standing relationships with qualified NEMT providers find that the operational friction around discharge transport decreases substantially. Drivers know the facility, intake procedures are streamlined, and the unpredictability of emergency dispatch is removed from an already complex discharge process.
Closing Perspective
The gap between ambulance services and non-emergency medical transport is not simply a question of cost or convenience. It reflects a more fundamental point about matching clinical resources to actual patient needs. Ambulances exist to respond to emergencies. Non-emergency transport, including rapid wheelchair & stretcher transport for patients with mobility limitations, exists to serve a large and underserved population whose needs are real, recurring, and entirely distinct from emergency medicine.
Making the right call requires knowing what each service is designed to do, what each one costs, and what outcomes each one reliably produces. For most stable patients with mobility limitations, the non-emergency option is not the lesser choice — it is the more appropriate, more efficient, and often more comfortable one. Care teams and families who understand this early in the transport planning process are better positioned to make decisions that actually serve the patient rather than simply satisfy an instinct toward caution.

